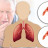
PROSTATITIS
1. What is prostatitis?
Prostatitis is a syndrome that presents with symptoms consistent with inflammation and/or infection of the prostate gland, including terminal dysuria, dysfunctional voiding, perineal pain, increased frequency of urination, and pain with ejaculation. Prostatitis is so common that up to 50% of all men may experience symptoms of this syndrome is their life time.
2. How is prostatitis classified?
Prostatitis is classified as bacterial or nonbacterial and is characterized as acute or chronic in nature.
3. What is prostadynia?
Patients with prostadynia have symptoms consistent with prostatitis , but cultures of prostatic secretions are negative and white blood cells are absent. The condition is theorized to occur secondary to bladder neck dysfunction (such as high tone or spasms), leading to reflux of urine into the prostatic and ejaculatory ducts.
4. How does acute bacterial prostatitis differ from chronic bacterial prostatitis?
Acute bacterial prostatitis
is usually a febrile illness of sudden onset, characterized by severe irritative symptoms, positive urine cultures, and a boggy, enlarged, and tender prostate on physical examination.
.
Chronic bacterial prostatitis
is characterized by persistent bacterial infections with inflammatory cells in prostatic secretions despite multiple regimens of prolonged antibiotic therapy. Patients typically have a long history of irritative symptoms, along with mild obstructive voiding.
5. How is prostatitis diagnosed?

It is difficult to diagnose prostatitis unless it is the acute bacterial variety. It is difficult to differentiate among chronic bacterial prostatitis, nonbacterial prostatitis, and prostadynia, because symptoms and physical findings may be similar.
6. What is the role of examination of prostatic secretions?
Prostatic secretions obtained by porstatic massage may reveal white blood cells from the initially voided specimen; bacterial may be seen in acute prostatitis.
7. What are segmented cultures or which portion of urine is collected ?
Segmented cultures are quantative cultures aimed at localizing bacteria to a particular segment of the urinary tract. Usually four segments are cultured. The first segment, called VB1, is the first voided 10 ml of urine. A positive VB1 culture indicates urethritis and/or prostatitis. A positive NB2 (midstream urine) culture indicates cystitis. EPS, or expressed positive cultures of VB3 ( first 10 ml of urine voided after prostatic massage), and expressed prostatic secretions (EPS) in dicate prostatic infection.
8. What is the most common pathogen in prostatitis?
Escherichia coli by far is the most common. Other agents include Enterobacter, proteus, Klebsiella, and Pseudomonas spp.
9. What are the most commonly used antibiotic agents in the treatment of prostatitis? Why?
The most commonly used agent is trimethoprim-sulfamethoxazole, given orally in a dose of 160-180 mg twice a day. In a sulfa-allegric patient, ciprofloxacin (a fluoroquinolone), 500 mg twice a day, is also an excellent choice. Both are superior to other agents because of their 2:1-3:1 concentration in prostatic tissue vs. serum.
10. How do treatment plans differ between acute and chronic prostatitis?
Acute prostatitis often presents with systemic manifestations. The involved pathogen is usually a gram-negative agent and may require parental administration of antibiotics, such as an aminoglycoside and ampicillin, followed by 4 week regimen of oral antibiotics to avert chronic bacterial prostatitis. Chronic bacterial prostatitis may require a prolonged antibiotic schedule. Patients often have prostatic calculi, which may harbor bacteria that present a potential for re-infection: chronic suppression may be required.
11. How is nonbacterial prostatitis treated?
Because no pathogen is isolated, a regimen of a broad-range antibiotic, such as doxycyline, may be tried. Patients with unsatisfactory results may be managed with anti-inflammatory agents. Some of these patients may respond to diet modification similar to that recommended for interstitial cystitis patients, i.e. , restricting caffeinated, acidic foods with emphasis on hydration.
12. How is prostadynia treated?
Prostadynia is by far the most difficult prostatic syndrome o treat: no infectious or inflammatory process is established. Patients are counseled on the nature of the syndrome, and treatment with an α-adrenergic agent and muscle relaxants, such as diazepam, has proved to be marginally successful. Previously mentioned dietary modification may also benefit these patients as they manage their symptoms.
13. What are the other forms of prostatitis?
Gonococcal prostatitis mycotic prostatitis
Tuberculous prostatitis nonspecific granulomatous prostatitis
Parasitic prostatitis
14. What is a prostatic abscess? How is it treated?
A prostatic abscess is a life-threatening infection of the prostate seen in immunocompromised patients, such as those with diabetes and renal failure. Treatment consists of immediate surgical drainage, including transurethral method and wide-spectrum parenteral antibiotics.
15. What other clinical diagnosis should be considered in patients with a history of acute or chronic prostatitis?
Some patients with a history of prostatitis refractive toconventional therapy should be considered for urodynamic evaluation . frequently , these patients have bladder dysfunction due to detrusor instability. The possibility of interstitial cystitis also should be considered if the patient does not respond to therapy.